If you’re a lover of walks or hikes, chances are that you’ve returned from your adventures feeling a little itchy at least once before. The outdoors are great. But it’s also home to many critters that have a knack for making themselves at home on your skin. Among these tiny hitchhikers is the black-legged tick, the culprit behind Lyme disease.
Commonly called deer ticks, black-legged ticks live on deer and other host animals like rodents and birds. The black-legged tick might seem harmless, but these ticks carry a bacterium called Borrelia burgdorferi. If you’re bitten by a deer tick infected with this bacterium, they can pass it on to you. That’s what causes Lyme disease. Let’s explore more about this disease, the signs and symptoms, treatment options, and ways you can protect yourself while still enjoying the great outdoors.
Lyme Disease on the Rise
The disease is most prevalent in areas with dense populations of deer ticks. These areas include the northeastern and upper midwestern United States, as well as parts of Europe, including the United Kingdom. In recent years, the incidence of Lyme disease has been on the rise in these areas. This is due to a number of factors including changes in land use, increasing deer populations, and climate change. These factors may sound arbitrary at first, but they all affect deer tick populations, which in turn affects likelihood of infection.

New cases are particularly emerging in suburban and peri-urban areas where human activities intersect with the habitat of deer ticks. Healthcare professionals, therefore, view Lyme disease as a growing public health concern. It is important for everyone to educate themselves on what this disease is, as well as the symptoms to look out for.
Early Lyme Disease Signs and Symptoms
Signs and symptoms of Lyme disease typically appear between 3 and 30 days after the initial infection. Here are some of the early symptoms.
Erythema migrans rash (Bull’s-eye rash)
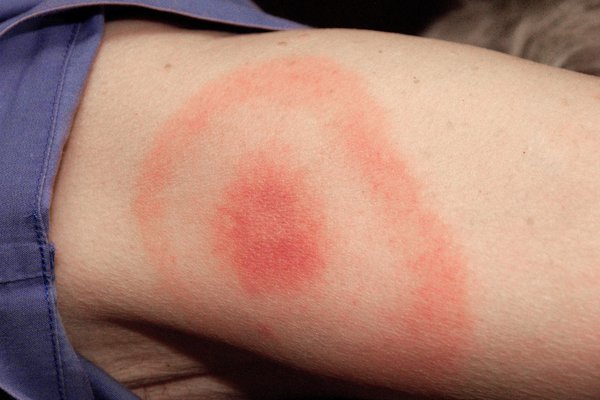
The Erythema Migrans (EM) rash is a hallmark early symptom of Lyme disease. For most Lyme disease patients, this is the first visible clue of infection. Also known as the bull’s-eye rash, this distinctive rash can be easy to spot. It is known as the bull’s-eye rash because of its appearance. It tends to look like a target – with a red dot at the site of the bite, surrounded by a central clearing and an outer ring of redness. While the bull’s-eye rash is well-known, the rash can also appear uniformly red, oval, or irregular in shape. The classic bulls-eye rash has been reported in about 60 to 80 %of Lyme disease cases, but remember many people do NOT get the rash.
EM rash gradually expands, sometimes reaching up to 11 inches (+/- 30cm) or more in diameter. It is usually painless, though it may feel warm to the touch. Recognizing this rash is critical for early diagnosis and treatment. If you notice an expanding rash after a tick bite, it is important to seek medical attention immediately.
Flu-like symptoms
In addition to the Erythema Migrans rash, flu-like symptoms are a common symptom of early-stage Lyme disease. These symptoms mimic the seasonal flu which can hinder early diagnosis. Most Lyme disease patients experience symptoms like fever, chills, fatigue, headaches, and swollen lymph nodes.
Unlike the flu, these symptoms do not resolve on their own and can worsen if left untreated. Recognizing the potential link between these flu-like symptoms and possible exposure to ticks is crucial for early intervention.
Muscle and joint pain
Joint aches, swelling and muscle aches are common symptoms of Lyme disease. These symptoms, known as Lyme arthritis, typically affect large joints such as the knees, but can also involve the hips, shoulders, and elbows. The affected joints may become inflamed, painful, and visibly swollen, sometimes with episodes of pain that can last from a few days to several weeks. This is because the bacteria – Borrelia burgdorferi can trigger an inflammatory response when it goes into the joint. Then, the immune system recognizes and starts to create a defence, leading to inflammation within the joint tissues. The tissues in the joint can then become infected.
Over time, you can develop Lyme arthritis. Symptoms can be intermittent, with periods of relative comfort followed by flare-ups of intense discomfort. In some cases, the joint pain may be misdiagnosed as other forms of arthritis, making it crucial to consider Lyme disease, especially if there has been potential exposure to ticks.
Prompt diagnosis and treatment with antibiotics are essential to manage these symptoms and prevent long-term joint damage.
Night sweats

Night sweats are notable symptoms of Lyme disease. They are your body’s natural response to try to fight the infection. Most Lyme disease patients experience intense night sweats, waking up drenched and uncomfortable. These sweats can disrupt their sleep patterns and contribute to overall fatigue. They may be accompanied by chills and fluctuating body temperatures.
Chronic Lyme Disease Symptoms
If left untreated, Lyme infections can spread to other parts of the body and cause chronic symptoms.
Once in the bloodstream, the bacteria Borrelia burgdorferi can cross the blood-brain barrier and invade the central nervous system (CNS). You may then develop an inflammatory response. The immune system reacts to the bacteria, causing inflammation around the brain—sometimes, the brain itself.
This can lead to a variety of neurological symptoms and signs, depending on the specific areas of the nervous system affected.
Along with the nervous system being infected, your joints or heart tissues can be affected by the bacteria.
Here’s a quick look at what those chronic symptoms might look like.
Neurologic symptoms
Chronic Lyme disease, when it reaches the nervous system, can lead to a variety of severe neurological symptoms, collectively known as Lyme neuroborreliosis. Patients may experience debilitating headaches, persistent neck stiffness, and episodes of Bell’s palsy, which is characterized by sudden facial drooping on one side.
Peripheral neuropathy is another common manifestation. It causes tingling, numbness, or sharp shooting pains in the extremities. In more advanced cases, the infection can result in meningitis, which involves inflammation of the membranes surrounding the brain and spinal cord, or encephalitis, leading to brain inflammation.
Neurologic Lyme disease complications can significantly impair a person’s quality of life, making early detection and aggressive treatment crucial to prevent long-term damage.
Cognitive decline
In addition to physical neurological symptoms, chronic Lyme disease often leads to notable cognitive decline. Patients frequently report experiencing “Lyme brain,” a term used to describe a variety of cognitive impairments. These can include difficulties with memory, such as forgetting recent conversations or misplacing items, and challenges with concentration, making it hard to focus on tasks or follow conversations. Information processing speed may also slow down, causing delays in understanding and responding to information.
This cognitive decline can interfere with daily activities, work performance, and social interactions, leading to increased frustration and stress. Addressing these cognitive symptoms typically involves a combination of medical treatment for the infection and supportive therapies, such as cognitive rehabilitation and mental health support, to help patients manage their condition and improve their quality of life.
Lyme carditis
This is a serious but less common manifestation of Lyme infection, occurring when the Borrelia burgdorferi bacteria infect the heart tissues. This condition can lead to inflammation of the heart, affecting its normal function and electrical conduction system. Patients with Lyme carditis may experience symptoms such as palpitations, chest pain, shortness of breath, lightheadedness, and even fainting.
Experiencing Early or Chronic Lyme Disease Symptoms?
If you think you have Lyme disease, it is essential to consult a healthcare professional as soon as possible. When you visit the doctor, you will be assessed, including a detailed medical history and physical examination. If you notice a rash or find a tick on your body, try to bring along pictures, as this can provide valuable information to your healthcare provider.
It’s likely, that your doctor will order blood tests to check for Lyme antibodies. This indicates the presence of the infection in your system. These blood tests not only help confirm a Lyme disease diagnosis but also assist in ruling out other conditions with similar symptoms, such as rheumatoid arthritis and other autoimmune diseases.
Prompt diagnosis and appropriate treatment with antibiotics are crucial for effectively managing Lyme disease and preventing more severe manifestations of the illness.
Treatment

Antibiotics are usually effective in the initial stage of Lyme disease. Early stages of Lyme disease are usually treated with oral antibiotics such as doxycycline, amoxicillin, or cefuroxime axetil [a doctor must prescribe]. These antibiotic courses are usually 2-4 weeks long. More severe cases may require intravenous antibiotics like ceftriaxone.
This, however, is not the case for people with ongoing/chronic Lyme disease symptoms such as fatigue, brain fog or musculoskeletal pains after an initial course of antibiotics. Antibiotics seem to be less effective, and symptoms are more advanced.
While some may experience short-term relief from antibiotics, according to the Infectious Diseases Society of America (IDSA), carefully performed clinical trials do not find the rates of improvement better than placebo. Watch this space, as more exciting research is currently in progress to find the best treatments!
Preventative Measures
It can be hard to avoid tick bites entirely, especially if you venture into woodsy areas often. But protecting yourself against Lyme disease can be as easy as doing some quick, smart preparation before you step outside. If you’re heading out to an area with a high population of deer tick:
- Apply insect repellent with at least 20% DEET on exposed skin and clothing. [ remember to check you are not allergic before use]
- Opt for light-coloured clothing to make it easier to spot any crawling intruders and make tick removal a breeze.
- Stick to well-maintained trails and avoid tall grasses and bushy areas where ticks are more likely to lurk to limit tick exposure.
- When you return, thoroughly check your body for ticks. Pay special attention to hidden areas like the scalp, behind the ears, under the arms, and around the waist.
By taking these precautions, you’re more likely to avoid tick bites. So you can enjoy your time in nature while minimizing the risk of Lyme disease.

How Long Does Lyme Disease Last?
The duration of a Lyme disease infection can vary significantly. If caught early and treated appropriately with antibiotics, most people recover fully within a few weeks. However, in some cases, symptoms can persist for months or even years. This leads to a condition often referred to as chronic Lyme disease or Post-Treatment Lyme Disease Syndrome (PTLDS).
PTLDS is characterized by persistent symptoms that continue in the long term, even after completing the standard antibiotic treatment for Lyme disease. Patients with PTLDS often experience ongoing fatigue, musculoskeletal pain, cognitive difficulties, and other flu-like symptoms. This can vary person to person though!
The exact cause of PTLDS is not well understood, and can therefore be challenging to manage, as there is currently no specific cure. Instead, treatment focuses on symptom relief and supportive care, including physical therapy, pain management, and cognitive rehabilitation. The condition significantly impacts patients’ quality of life, and continued research aims to understand its mechanisms better and develop more effective treatment strategies.
Can Lyme Disease Be Fatal?
Lyme disease is rarely fatal. However, complications from the disease, such as severe cardiac or neurological involvement, can be serious if not treated promptly. Not sure if you’re exhibiting the symptoms? It’s always better to play it safe and consult a doctor so we can address you concerns.
Is Lyme Disease Contagious?
Lyme disease is not contagious and cannot be transmitted from person to person through casual contact. The primary mode of transmission is through the bite of an infected tick carrying the Borrelia burgdorferi bacteria.
While Lyme disease cannot spread through human contact, it is important to be aware that infected ticks can attach to clothing, pets, or outdoor gear, potentially leading to further bites or bringing ticks into your home. Preventive measures, such as using insect repellent on exposed skin and clothing, performing regular tick checks, and promptly removing any attached ticks, are essential to reduce the risk of Lyme disease.
Misdiagnosis: Nummular Eczema

Lyme disease and nummular eczema both have rashes that may be easily confused due to their similar appearance. Lyme disease typically manifests a rash that looks like a circular, red patch with a clear centre, resembling a bull’s eye. In contrast, nummular eczema presents as round, coin-shaped patches of irritated skin that can be red, scaly, and itchy. These patches are often mistaken for the Lyme disease rash due to their round shape and inflamed appearance.
While these rashes may look similar, the key to differentiating between the two lies in understanding the symptoms associated with each. Lyme disease is often accompanied by flu-like symptoms, while nummular eczema is a chronic condition often triggered by dry skin, allergens, or irritants.
If you have a rash that you’re struggling to identify – your doctor will support you with diagnosis, advice and treatment.
Misdiagnosis: Fibromyalgia

A common misdiagnosis of Lyme disease is fibromyalgia, a chronic condition characterized by widespread musculoskeletal pain, fatigue, and cognitive difficulties. Both share similar symptoms such as joint pain, muscle aches, and severe fatigue, which can lead to confusion in diagnosis. However, while Lyme disease is caused by the bacterium Borrelia burgdorferi transmitted through tick bites, fibromyalgia’s exact cause remains unclear but is often associated with abnormal pain processing in the brain.
A misdiagnosis can result in inappropriate treatment, as fibromyalgia is typically managed with pain relievers, antidepressants, and lifestyle changes, whereas Lyme disease requires antibiotic therapy.
Key Takeaways
Lyme disease is a complex illness passed to humans via black-legged ticks, also called deer ticks.
Since deer ticks carry the bacterium that causes Lyme infection, taking a few quick precautions before heading into deer tick-dense territory can lower your risk of being infected.
The impact of Lyme disease on quality of life can be significant, particularly if it progresses to a chronic stage.
Awareness of the signs and symptoms, and early intervention are critical to managing the disease effectively.
Watch my quick video guide on this infectious disease:
Disclaimer: The Content on this channel is for educational purposes and not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always get advice from your doctor if you are worried or have symptoms.